- Max Healthcare
- drbhamrinaveen@rediffmail.com
- 8802154156, 8285815017
- Max Healthcare
- drbhamrinaveen@rediffmail.com
- 8802154156, 8285815017
Coronary interventions are specialized, minimally invasive procedures used to treat Coronary Artery Disease (CAD). CAD occurs when the arteries that supply blood to the heart muscle become narrowed or blocked by a buildup of plaque (fat, cholesterol, and other substances).
Commonly known as Percutaneous Coronary Intervention (PCI) or Angioplasty, these procedures are designed to open clogged heart arteries. Unlike open-heart surgery, these interventions are performed through a small puncture, usually in the groin or wrist, using thin, flexible tubes called catheters.
The primary goal is to improve blood flow to the heart, relieve symptoms like chest pain (angina), and reduce the risk of a heart attack.
While the basic goal remains opening a blocked artery, the “how” has become significantly more precise:
Fractional Flow Reserve (FFR): Before treating a blockage, doctors often use a pressure-sensing wire to measure the actual blood flow across a narrowing. This ensures that only blockages that are truly restricting oxygen to the heart are intervened upon.
Intravascular Imaging: Modern interventions often use IVUS (Intravascular Ultrasound) or OCT (Optical Coherence Tomography). These are tiny cameras or sensors inside the artery that provide a 360-degree view of the plaque. This allows for perfect stent sizing and placement.
Depending on the type of blockage, different tools may be used:
Drug-Eluting Stents (DES): These are the gold standard. The mesh is coated with medication that is released over several weeks to prevent “restenosis” (the growth of scar tissue that could re-block the artery).
Rotational Atherectomy: For blockages that are very hard or “calcified,” a tiny, diamond-tipped drill (rotablator) is used to gently shave away the calcium before a stent is placed.
Lithotripsy (Shockwave): Similar to how kidney stones are treated, sound waves can be used to crack hard calcium within the artery wall to allow the vessel to expand safely.
The “what” of these interventions extends beyond just fixing a physical pipe. They are critical for:
Myocardial Salvage: In the event of an acute heart attack, “time is muscle.” Every minute saved in performing a coronary intervention preserves more of the heart’s pumping function.
Ischemia Management: For chronic patients, these procedures transform quality of life by allowing them to walk, climb stairs, and exercise without the crushing weight of chest pain.
Success depends heavily on what happens after the patient leaves the lab:
Dual Antiplatelet Therapy (DAPT): Patients must take blood-thinning medications for a specific period to prevent blood clots from forming on the new stent.
Cardiac Rehabilitation: A structured program of exercise and education to strengthen the heart and manage underlying risk factors like high blood pressure or cholesterol.
Balloon Valvuloplasty (also called balloon dilation) is a specialized procedure used to treat a stenotic valve—a condition where a heart valve becomes stiff, scarred, or fused, preventing it from opening fully. When a valve is narrowed (stenosed), the heart must work significantly harder to pump blood through the smaller opening.
In a healthy heart, valves act as one-way gates that open wide to let blood flow through. In stenosis:
The valve leaflets (flaps) become thick or calcified.
The opening narrows, restricting blood flow.
This can lead to fatigue, shortness of breath, chest pain, and eventually heart failure.
Balloon valvuloplasty is a percutaneous (through the skin) procedure, meaning it does not require opening the chest. It is often used for the mitral, aortic, or pulmonary valves.
A thin, flexible tube (catheter) is inserted through a blood vessel, usually in the groin. Using real-time X-ray imaging (fluoroscopy), the cardiologist guides the catheter up into the heart and positions it precisely within the narrowed valve.
Placement: A specialized deflated balloon at the tip of the catheter is placed across the stiff valve leaflets.
Inflation: The doctor quickly inflates the balloon. The force of the inflation stretches the valve opening and separates the leaflets that have become fused or stuck together.
Verification: The balloon is deflated and inflated several times to ensure the opening is sufficiently widened.
Once the valve is sufficiently opened, the balloon is deflated and removed along with the catheter. The valve can now open more freely, restoring better blood flow and reducing the workload on the heart muscle.
While some cases eventually require a full valve replacement, balloon dilation offers several advantages:
Minimally Invasive: No large incisions or use of a heart-lung machine.
Shorter Recovery: Most patients stay in the hospital for only one night and return to normal activities within days.
Effective Bridge: It is an excellent option for children with congenital stenosis or for elderly patients who may be too frail for open-heart surgery.
Following the dilation, patients typically experience immediate improvement in symptoms. Long-term care involves:
Follow-up Echo: An echocardiogram (ultrasound) is usually performed to measure the new valve area and ensure blood is flowing correctly.
Monitoring: While highly effective, some valves may narrow again over time (restenosis), requiring further monitoring or future intervention.
Peripheral vascular disease (PVD) is a blood circulation disorder that causes the blood vessels outside of your heart and brain to narrow, block, or contract. This can happen in your arteries or veins. It can also affect the vessels that supply blood and oxygen to your arms, stomach & Intestines and kidneys. For many people, the first signs of PVD begin slowly and irregularly. You may feel discomfort like fatigue and cramping in your legs and feet that gets worse with physical activity due to the lack of blood flow.
Peripheral Vascular Disease (PVD) is a medical condition affecting blood vessels outside the heart and brain. It is characterized by the narrowing, blockage, or damage of arteries and veins in the extremities, such as the legs and arms. PVD is mainly associated with atherosclerosis, a process in which fatty deposits called plaques build up in the walls of blood vessels, causing them to become narrower and less flexible.
As the arteries and veins become restricted, blood flow to the affected areas is reduced, leading to various health complications. PVD can cause discomfort, pain, and limited mobility. If left untreated, it may result in more severe consequences, such as non-healing wounds, infections, and in extreme cases, tissue death (gangrene).
To comprehend Peripheral Vascular Disease (PVD) and the significance of peripheral artery disease surgery, it’s essential to understand the circulatory system’s role in the body. The circulatory system, also known as the cardiovascular system, plays a vital role in transporting blood throughout the body. It consists of the heart, blood vessels, and blood.
The heart serves as a powerful pump, pushing oxygen-rich blood from the lungs into the arteries, which carry this oxygenated blood to various parts of the body. As the tissues use up oxygen and nutrients, the blood becomes depleted of oxygen and returns to the heart through the veins to be reoxygenated.
However, in the context of PVD, the condition affects the blood vessels responsible for carrying blood away from the heart to the extremities. The buildup of plaques in these vessels narrows the passageway, restricting the smooth flow of blood. This reduced blood flow leads to decreased oxygen and nutrient supply to the tissues and muscles in the affected areas. Consequently, individuals with PVD may experience pain, cramping, weakness, and difficulty walking or performing everyday activities.
PVD is closely associated with other cardiovascular risk factors, such as high blood pressure, high cholesterol levels, and diabetes. Moreover, it often coexists with coronary artery disease (CAD), which affects the blood vessels supplying the heart. As such, managing PVD becomes crucial to improve limb function and enhance the quality of life and reduce the risk of heart-related complications.
For effective management of PVD, early diagnosis and appropriate treatment are imperative. Dr. Naveen Bhamri, Head of Department & Senior Director of Interventional Cardiology at Max Super Speciality Hospital in North & West Delhi, offers specialized care in peripheral artery disease surgery. His expertise enables him to provide personalized treatment plans and state-of-the-art interventional cardiology procedures to restore blood flow and enhance overall vascular health.
Understanding the impact of PVD on the circulatory system empowers individuals to take proactive steps in managing their vascular health and leading healthier, more active life through timely intervention and guidance from experts like Dr. Naveen Bhamri. Patients can significantly improve their outcomes and prevent further progression of the disease. By incorporating peripheral artery disease surgery, Dr. Bhamri’s comprehensive approach ensures the best possible results for those seeking relief from PVD symptoms and a better quality of life.
Peripheral Vascular Disease (PVD) is a complex condition influenced by various factors. Among the leading causes are lifestyle choices and underlying health conditions. Understanding these contributing elements is vital for early detection and prevention. It is essential to seek guidance from experts such as Dr. Naveen Bhamri, a distinguished peripheral vascular doctor in India, and his team comprises interventional cardiologist and vascular surgeon.
Smoking is a significant risk factor for PVD. The harmful chemicals in tobacco can damage the blood vessels, promoting the development of atherosclerosis and increasing the likelihood of plaque buildup. Dr. Naveen Bhamri emphasizes the importance of quitting smoking to reduce the risk of PVD and its associated complications.
Individuals with diabetes are at higher risk of developing PVD due to the impact of elevated blood sugar levels on blood vessel health. Diabetes can accelerate atherosclerosis and impair blood flow, particularly in the lower extremities. Regular monitoring and proper management of diabetes are essential to minimize the risk of PVD.
Uncontrolled high blood pressure (hypertension) stresses the blood vessel walls, making them more susceptible to damage and plaque formation. Maintaining a healthy blood pressure level is crucial for reducing the risk of PVD and its progression.
Elevated levels of cholesterol, especially low-density lipoprotein (LDL) cholesterol, can lead to the buildup of fatty deposits in the blood vessels. These deposits contribute to atherosclerosis, narrowing the arteries and reducing blood flow to the extremities. If necessary, managing cholesterol levels through diet, exercise, and medication is essential for PVD prevention.
Lack of physical activity can lead to various health issues, including obesity and impaired circulation. Engaging in regular exercise helps maintain healthy blood vessels, improves blood flow, and reduces the risk of PVD. Dr. Naveen Bhamri, a renowned peripheral vascular doctor in India, and his team of interventional cardiologist and vascular surgeons advocate for an active lifestyle as a preventive measure against PVD.
Smoking is a significant risk factor for PVD. The harmful chemicals in tobacco can damage the blood vessels, promoting the development of atherosclerosis and increasing the likelihood of plaque buildup. Dr. Naveen Bhamri emphasizes the importance of quitting smoking to reduce the risk of PVD and its associated complications.
Individuals with diabetes are at higher risk of developing PVD due to the impact of elevated blood sugar levels on blood vessel health. Diabetes can accelerate atherosclerosis and impair blood flow, particularly in the lower extremities. Regular monitoring and proper management of diabetes are essential to minimize the risk of PVD.
Uncontrolled high blood pressure (hypertension) stresses the blood vessel walls, making them more susceptible to damage and plaque formation. Maintaining a healthy blood pressure level is crucial for reducing the risk of PVD and its progression.
Elevated levels of cholesterol, especially low-density lipoprotein (LDL) cholesterol, can lead to the buildup of fatty deposits in the blood vessels. These deposits contribute to atherosclerosis, narrowing the arteries and reducing blood flow to the extremities. If necessary, managing cholesterol levels through diet, exercise, and medication is essential for PVD prevention.
Lack of physical activity can lead to various health issues, including obesity and impaired circulation. Engaging in regular exercise helps maintain healthy blood vessels, improves blood flow, and reduces the risk of PVD. Dr. Naveen Bhamri, a renowned peripheral vascular doctor in India, and his team of interventional cardiologist and vascular surgeons advocate for an active lifestyle as a preventive measure against PVD.
Dr. Naveen Bhamri, a renowned coronary interventional cardiologist in India, offers advanced peripheral artery disease surgery at Max Super Speciality Hospital. His expertise and state-of-the-art procedures give patients personalized care and improved vascular health. By addressing risk factors and adopting a proactive approach, individuals can lead a healthier, more active life while effectively managing PVD and related conditions.
A pacemaker is a sophisticated medical device that regulates and stabilizes the heart’s rhythm. It is a small, battery-powered device that is surgically implanted under the skin, typically in the chest area, just below the collarbone, best doctor for pacemaker. The pacemaker is connected to one or more leads (thin wires) that are carefully threaded through the veins and attached to specific locations within the heart.
The primary function of a pacemaker is to monitor the heart’s electrical activity continuously. When the pacemaker detects abnormal heart rate or rhythm, it automatically sends electrical signals to the heart, prompting it to beat correctly. This ensures the heart maintains an optimal rhythm, pumps blood effectively, and distributes oxygen and nutrients throughout the body.
Pacemakers are instrumental in managing various heart conditions, particularly irregular heartbeats (arrhythmias) or bradycardia, which is an abnormally slow heart rate. A pacemaker can prevent symptoms such as dizziness, fainting, and fatigue by providing timely electrical stimulation, thereby significantly improving the overall quality of life for individuals with heart rhythm disorders.
A pacemaker is needed to keep track of your heart rate and stimulate it to beat faster. While pacemakers are not used to treat all heart diseases or irregular heartbeats, there are several symptoms that indicate who needs one. If you notice any of these symptoms, make an appointment with your doctor for a checkup.
Pacemaker implantation becomes necessary for individuals with specific heart conditions that affect the heart’s rhythm and electrical activity. Some common heart conditions that may require a pacemaker include:
Individuals experiencing certain symptoms may need a pacemaker to regulate their heart rhythm effectively. These symptoms may include:
Palpitations: Sensations of rapid, irregular, or pounding heartbeats could indicate arrhythmias that may benefit from a pacemaker’s corrective measures.
Timely diagnosis and intervention are crucial when considering pacemaker implantation. Seeking consultation with the best doctor for pacemaker-related concerns, such as a cardiologist pacemaker specialist in Delhi, ensures accurate evaluation and appropriate treatment recommendations.
Delaying pacemaker implantation can lead to worsening symptoms and an increased risk of complications. A timely diagnosis allows for effective management of heart conditions, enabling patients to lead healthier, more active lives.
Dr. Naveen Bhamri, a renowned cardiologist pacemaker specialist in Delhi, practicing at Max Super Speciality Hospital, offers comprehensive assessments and personalized treatment plans for individuals requiring pacemaker support. His expertise in the field ensures that patients receive the most appropriate intervention at the right time, leading to improved heart function and enhanced overall well-being. Seeking timely medical attention and guidance from experts like Dr. Bhamri is vital in maintaining heart health and managing heart rhythm disorders effectively.
Dr. Naveen Bhamri, a renowned pacemaker implantation surgeon, is committed to providing the highest level of care to patients with various heart rhythm disorders.
Dr. Naveen Bhamri, the best doctor for pacemaker, specializes in the implantation of various pacemakers tailored to meet individual patient needs. Whether single-chamber or dual-chamber pacemakers, our skilled team ensures precise and successful pacemaker implantation procedures. Pacemakers play a crucial role in regulating the heart’s rhythm, ensuring optimal blood flow, and improving the overall quality of life for patients with bradycardia or heart block.
Dr. Naveen Bhamri, a top pacemaker implantation surgeon, also offers Cardiac Resynchronization Therapy (CRT) for patients with heart failure and electrical conduction issues. CRT – P (CRT – Pacemaker) and CRT – D (CRT – Defibrillator) are specialized devices that help synchronize the heart’s contractions, improving pumping efficiency and reducing heart failure symptoms. Our expert team performs these advanced procedures to relieve and enhance cardiac function for eligible patients.
Automatic Implantable Cardioverter-Defibrillators (AICDs) are life-saving devices that monitor heart rhythms and deliver electrical shocks if life-threatening arrhythmias are detected. Our skilled surgeons perform implantations of single and dual-chamber AICDs, ensuring patients have the best protection against sudden cardiac events.
Dr. Naveen Bhamri and his team offer advanced and comprehensive care for individuals requiring pacemaker implantation surgery in India. With years of experience in heart pacemaker surgery, Dr. Bhamri is dedicated to providing personalized treatment plans and state-of-the-art procedures. At Max Super Speciality Hospital, patients expect world-class facilities, cutting-edge technology, and a patient-centric approach, ensuring the best possible outcomes for pacemaker implantation surgery in India.
Whether single-chamber or dual-chamber heart pacemaker surgery, Dr. Naveen Bhamri’s expertise guarantees precise diagnoses and effective interventions, leading to improved heart function and a better quality of life for patients requiring pacemaker support.
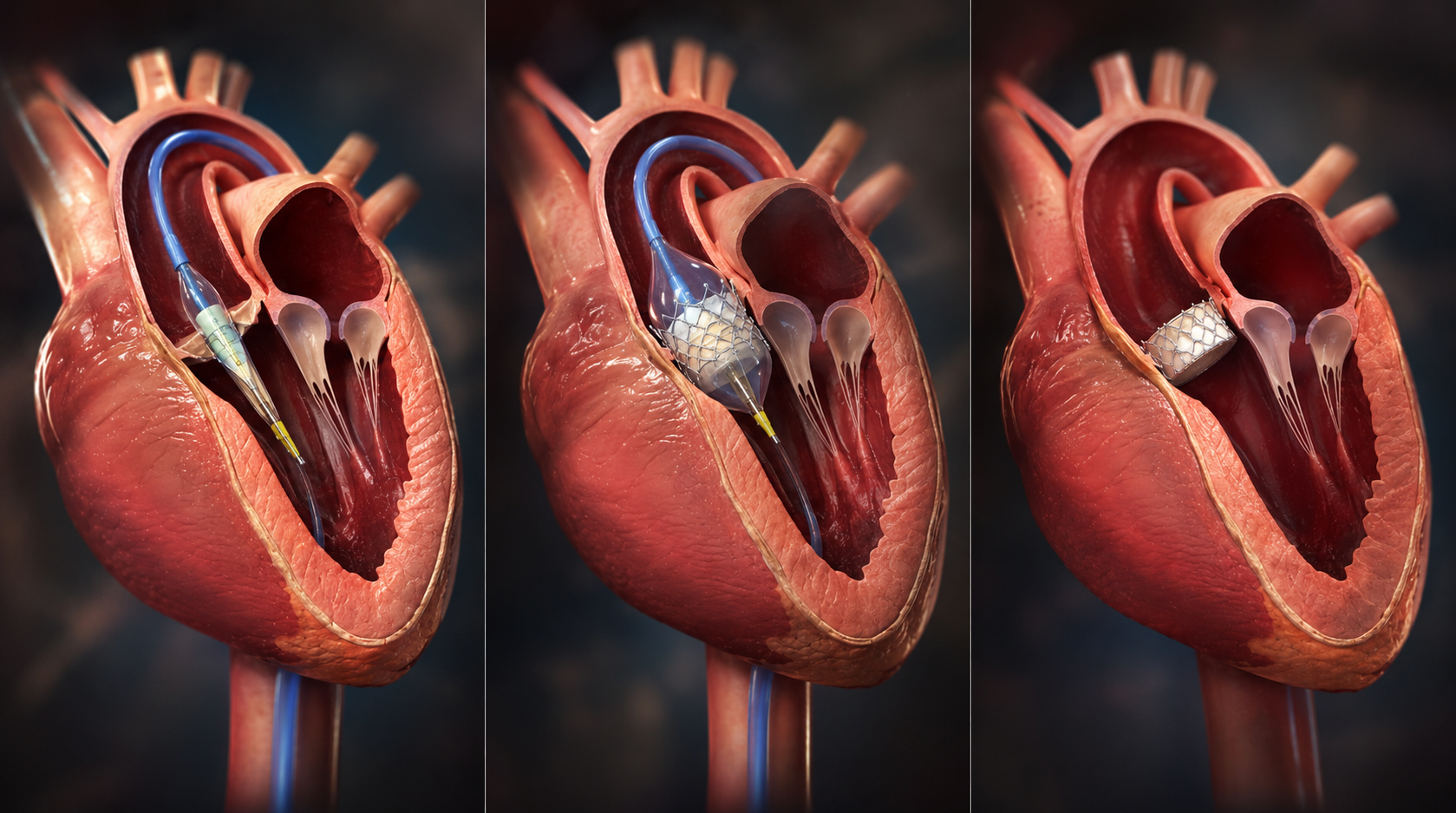
TAVI, also known as TAVR (transcatheter aortic valve replacement), is a new technology to treat severe aortic stenosis, a less invasive procedure, designed to replace a diseased aortic valve. Until now, the only treatment for patients with aortic stenosis was surgically replacing the aortic valve by undergoing an open-heart surgery. However, there are about 40% of patients who are refused a surgery due to their co-morbid conditions. The surgical procedures are invasive, take longer to perform and the recovery from surgery can take up to three to eight weeks.
TAVI/TAVR is a good alternative for these high-risk groups of patients. In this method, via a small cut in the groin a thin, flexible tube with the heart valve is inserted into your artery and up to your diseased valve. Throughout the procedure, the doctor views images of the heart and the valve is replaced, and the new valve works immediately. The tube is then removed, and the incision is closed. The entire procedure takes approximately one to two hours.
Many patients’ quality of life has greatly improved due to TAVI Valve Implantation in India. Most patients find a reduction in their symptoms following a TAVI surgical operation, improving their capacity to carry out everyday tasks. It is important to understand that problems are a possibility with any medical procedure. However, you can make a full recovery if you work with the best transcatheter aortic valve implantation doctors like Dr. Naveen Bhamri.
Incorporating healthy lifestyle changes is highly beneficial to enhance the chances of achieving long-term success and reduce the risks associated with TAVI. Some critical lifestyle adjustments include:
By taking these proactive steps, you can optimize the success of your TAVI transaortic valve implantation in Delhi and contribute to a healthier and more fulfilling life.
Meet Dr. Naveen Bhamri, one of the best heart specialist doctors, a distinguished and highly skilled cardiologist renowned for his Transcatheter Aortic Valve Implantation expertise. With a passion for delivering outstanding patient care and a commitment to pushing the boundaries of cardiovascular medicine, Dr. Bhamri stands at the forefront of TAVI procedures.
Expertise and Experience: Dr. Naveen Bhamri is a leading cardiologist. He has a proven track record of effective procedures and has accumulated priceless experience that allows him to confidently and correctly handle even the most challenging instances.
Compassionate Patient Care: At the heart of Dr. Bhamri’s practice is his unwavering commitment to providing personalized and compassionate care to every patient. He takes the time to understand each individual’s unique medical history and concerns, ensuring a tailored approach to treatment.
Modern Technology: Dr. Naveen makes it a point to stay updated on cardiovascular medicine’s most recent developments. To give the best results and improve patient safety, he makes use of the latest technologies and does the work of peripheral vascular surgeons as well.
Patient Education: Dr. Naveen Bhamri firmly believes in empowering patients with knowledge. He takes the time to explain the TAVI procedure in detail, addressing any concerns and guiding patients and their families throughout the treatment journey.